|
13, 14 Fewer studies have looked at the larger range of health-related outcomes including cost and the provider experience, or at which attributes effective interventions might have in common. 7, 8, 9, 10 Previous reviews have explored the effectiveness of resulting interventions, 11, 12 mostly focusing on how they might improve patient morbidity and satisfaction with care. 6Įfforts to improve interpersonal patient–provider interactions have often used patient-centered approaches (e.g., shared decision-making) to enhance communication. 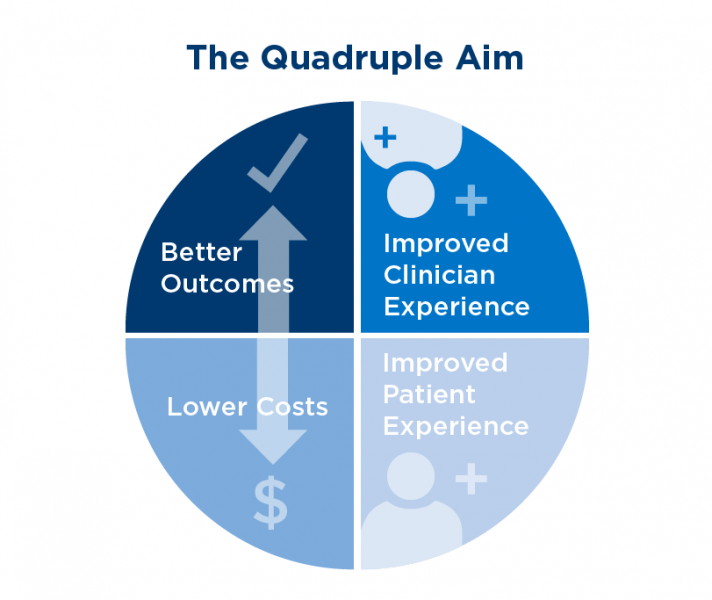
3, 4, 5 Moreover, routinely failing to connect contributes to physician burnout, which may initiate a downward spiral in patient–provider relationships. 1, 2 Beyond their inherent value, better connections between patients and providers can improve symptoms, increase adherence to medical recommendations, and reduce medical errors. Humanism is central to clinical care, yet the demands of modern medicine and technology can interfere with meaningful interpersonal interactions between patients and providers. Simple, low-demand patient–provider interpersonal interventions may have the potential to improve patient health and patient and provider experience, but there is limited evidence that these interventions influence cost-related outcomes. Interventions with lower demands on provider time and effort were often as effective as those with higher demands. Among studies that measured time in the clinical encounter, intervention effects varied. Roughly a quarter of studies evaluated cost, but the majority reported no significant differences between intervention and control groups. Enhanced interpersonal interactions improved provider well-being, burnout, stress, and confidence in communicating with difficult patients. Most studies measured impact on patient experience improvements in experience (e.g., satisfaction, patient-centeredness, reduced unmet needs) often corresponded with a positive impact on other patient health outcomes (e.g., quality of life, depression, adherence). The methodological quality of research was moderate to high for most included studies 67% of interventions targeted the provider. Seventy-three out of 21,835 studies met the design and outcome inclusion criteria. provider–patient dyad), and quadruple aim outcomes. We characterized evidence related to the objective of the intervention, type and duration of intervention training, target recipient (provider-only vs. Two abstractors independently extracted information about study design, methods, and quality. 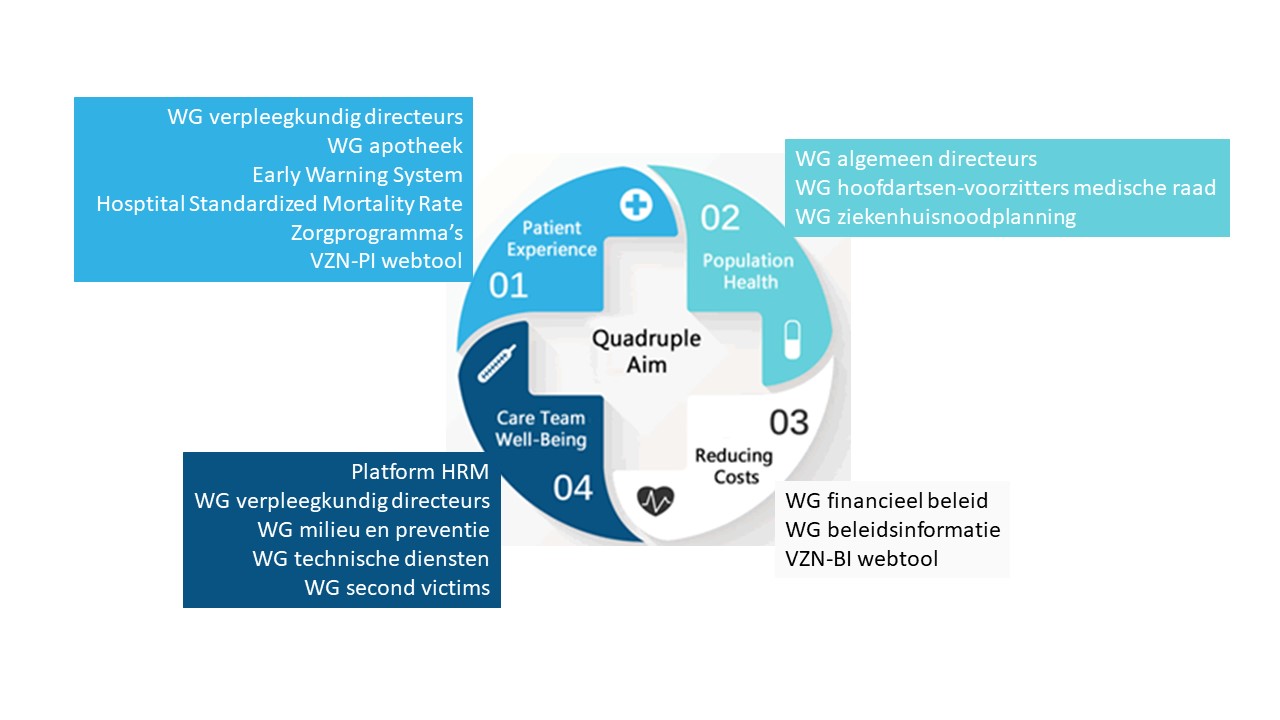
Selected studies included randomized controlled trials and controlled observational studies that examined the association between patient–provider interpersonal interventions and at least one outcome measure of the quadruple aim. We sourced data from PubMed, EMBASE, and PsycInfo (January 1997–August 2017). The purpose of this review was to characterize the associations between patient–provider interpersonal interventions and the quadruple aim outcomes (population health, patient experience, cost, and provider experience). 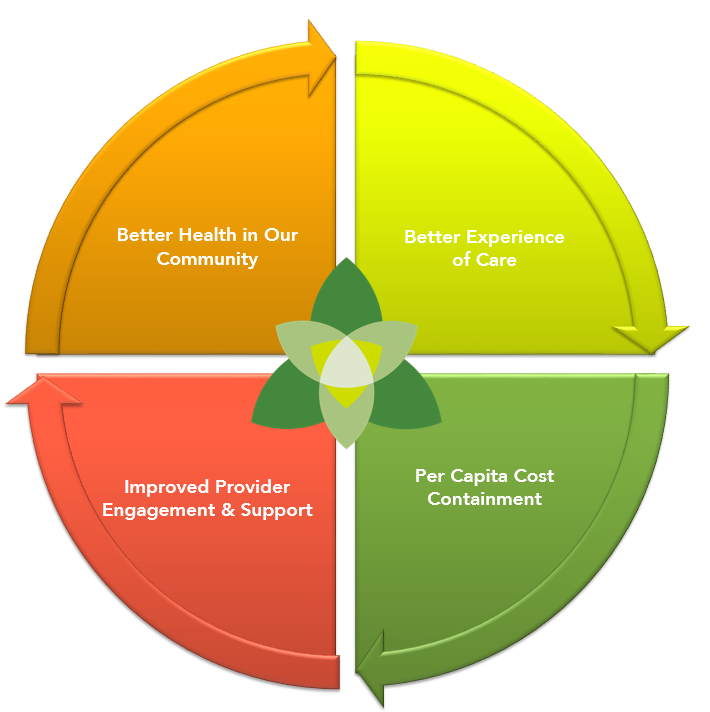
Human connection is at the heart of medical care, but questions remain as to the effectiveness of interpersonal interventions.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
